Pioneer in Offering CRM Solutions since 2010...
Pioneer in Offering CRM Solutions since 2010...

Set desired parameters & eEligibility will automatically check carrier benefits for the upcoming appointments in your scheduling system.
Coverage info automatically feeds into the patient scheduler, appointment screen, insurance tab, patient memo & summary report.

eEligibility will create a memo & automatically notify you of any charges that aren’t covered by a patient’s current benefits plan.
Dental plans are complex, have many exclusions,waiting periods, alternate benefits and tricky benefit wording to add to the confusion. Incorrect insurance verifications can affect many unexpectedoutcomes that include high account receivables, low collection, outstanding claims, frustrated patients and myriad of challenges in reimbursement.
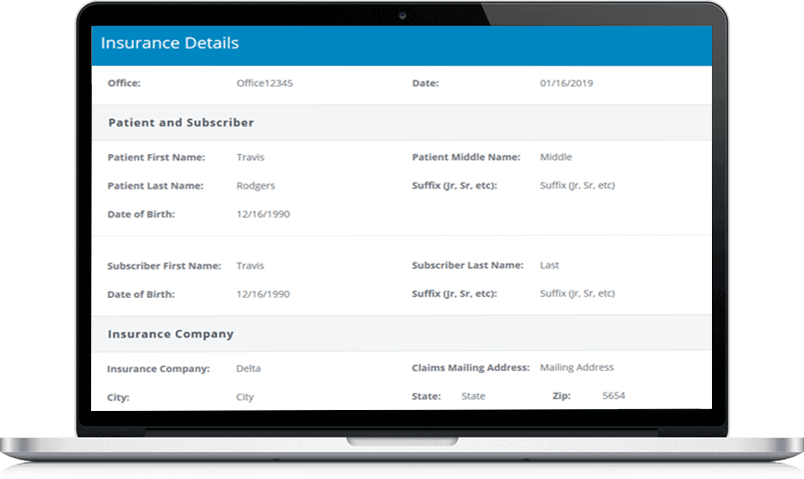
All challenges can be avoided by having simply verified patient’s benefits prior to their appointment. Our verification app mitigate your worries by ensuring that insurance verification will be done by one simple click. With this information the patient will be greeted with an accurate coverage amount and estimated copayment, which results in a loyal, happier and trusting patient.
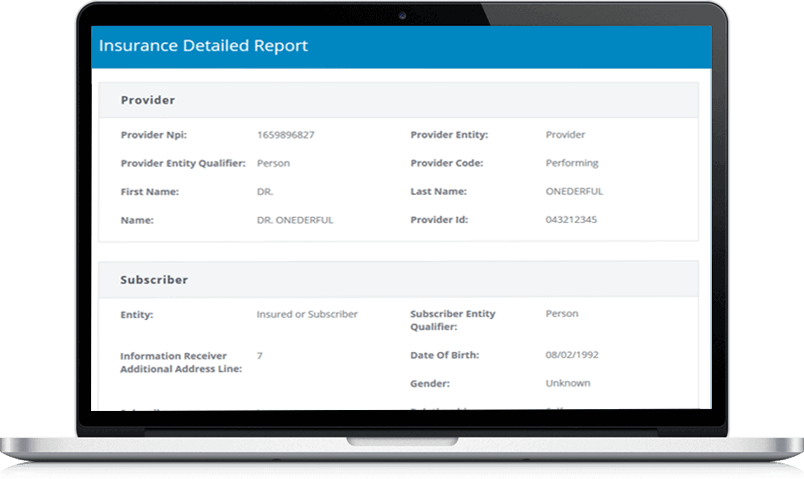
.png)










Angular 7, Asp.net WebAPI 2.0

SQL server-2017

Bootstrap4, Angular-Material.

Mandrill, Onederful
Variance InfoTech Pvt Ltd.
608/609, 6th floor - Abhishree Adroit,
Vastrapur, Ahmedabad, 380015, India
For Sales: +91-7016851729
For Job Inquiry: +91 98700 57291
Email : info@varianceinfotech.in
Variance InfoTech LLC
30 N Gould St. Sheridan,
WY 82801 USA
Phone: +16305340223
Email: info@varianceinfotech.in
All product names, logos, and brands are property of their respective owners. Use of these names, logos, and brands does not imply endorsement.
©Copyright 2026. All Rights Reserved | Privacy Policy
We use cookies to provide better experience on our website. By continuing to use our site, you accept our Cookies and Privacy Policy.
Accept





